The Problem of Lower Back Pain: Causes, Diagnosis & Modern Management
Lower back pain is one of the most common health complaints worldwide. A sudden twist, lifting a heavy object incorrectly, or even getting out of bed the wrong way can leave a person immobilized with severe discomfort. For many adults, it becomes a recurring issue that affects productivity, sleep, and overall quality of life.
According to global health estimates, lower back pain is among the leading causes of work absenteeism and disability. Fortunately, most cases are manageable with timely diagnosis, appropriate treatment, and lifestyle correction.
How Lower Back Pain Affects Mobility
The lower back (lumbar spine) supports most of the body’s weight. It allows bending, twisting, lifting, and maintaining posture. The spinal column protects delicate nerve roots that transmit signals between the brain and the lower body.
When inflammation, muscle strain, or disc compression occurs, mobility becomes restricted. Patients may find it difficult to:
Bend forward
Stand for long periods
Sit comfortably
Walk without pain
If nerve roots are compressed, pain may radiate to the buttocks or legs — a condition commonly known as sciatica.
Common Symptoms of Lower Back Pain
Patients may experience:
Persistent muscle soreness
Sudden sharp or shooting pain
Pain radiating to one or both legs
Worsening discomfort with movement
Relief while reclining or leaning backward
Stiffness, especially in the morning
Red flag symptoms requiring urgent evaluation:
Loss of bladder or bowel control
Progressive weakness in legs
Fever with back pain
History of trauma
Major Causes of Lower Back Pain
1. Muscle or Ligament Strain
Sudden movements, improper lifting techniques, or repetitive strain can overstretch muscles and ligaments. Poor physical conditioning increases susceptibility.
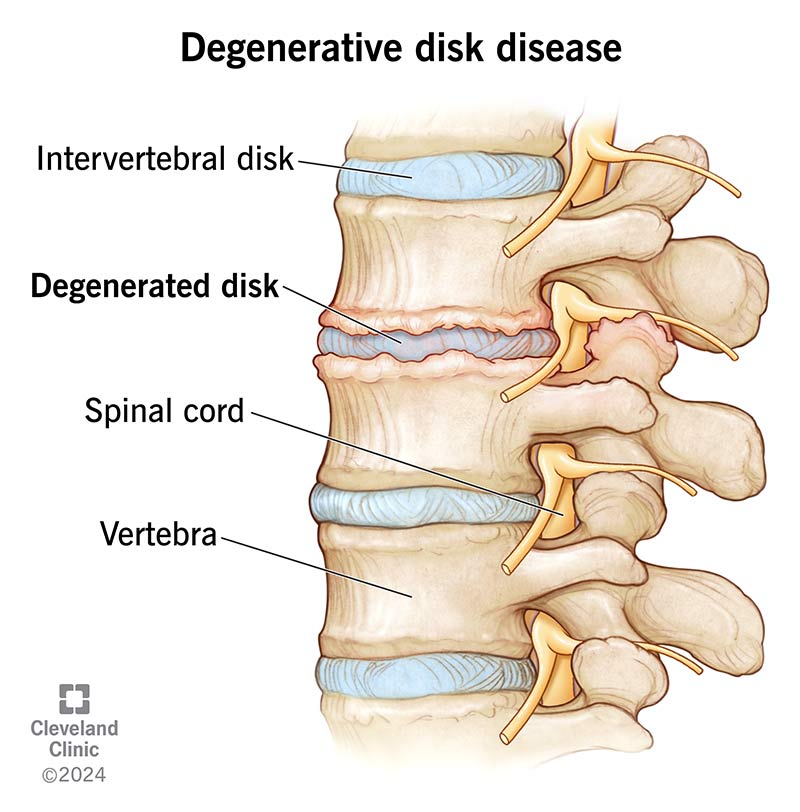
2. Disc Degeneration or Herniation
Intervertebral discs act as cushions between vertebrae. With age or stress, discs may:
Bulge
Herniate
Lose hydration
This can compress nerves and cause radiating pain.
3. Arthritis
Conditions such as osteoarthritis can narrow spinal spaces (spinal stenosis), leading to nerve compression.
4. Skeletal Abnormalities
Spinal curvature disorders (like scoliosis) can disrupt alignment and cause chronic discomfort.
5. Osteoporosis
Weak bones may develop microfractures, especially in elderly individuals.
Diagnostic Evaluation
Proper medical evaluation is essential to determine the underlying cause.
X-ray
Useful for detecting fractures, alignment issues, and bone degeneration.
MRI Scan
Provides detailed images of discs, nerves, and soft tissues. Ideal for diagnosing herniated discs and nerve compression.
Electromyography (EMG)
Assesses nerve function and muscle response, especially in suspected nerve damage cases.
Treatment Options
Treatment depends on the cause, severity, and duration of pain.
1. Medications
NSAIDs (e.g., ibuprofen) for inflammation
Muscle relaxants for spasms
Short-term opioids in severe cases (under strict supervision)
Topical analgesic creams
2. Physiotherapy
Structured physiotherapy improves flexibility, strengthens muscles, and reduces recurrence.
3. Posture Correction
Maintain upright sitting posture
Use lumbar support
Avoid prolonged sitting
Adjust workstation ergonomics
4. Core Strengthening Exercises
Strong abdominal and back muscles stabilize the spine. Recommended exercises include:
Pelvic tilts
Bridges
Planks
McKenzie extension exercises
5. Massage & Manual Therapy
Therapeutic massage improves circulation and reduces muscle tension. Some patients benefit from spinal manipulation performed by trained professionals.
6. Sleep Optimization
Sleep on the side with a pillow between knees
Use a medium-firm mattress
Avoid stomach sleeping
Sciatica: A Special Consideration
Sciatica occurs when the sciatic nerve is compressed, usually due to disc herniation. Symptoms include:
Shooting pain from lower back to leg
Tingling or numbness
Burning sensation
Management includes:
Anti-inflammatory medication
Physiotherapy
Nerve mobilization exercises
Epidural steroid injections (in selected cases)
Surgery (rare, severe compression cases)
Prevention Strategies
✔ Maintain healthy body weight
✔ Exercise regularly (especially core strengthening)
✔ Avoid sudden jerky movements
✔ Lift objects using knees, not the back
✔ Quit smoking (improves disc health)
✔ Ensure adequate calcium and vitamin D intake
When to See a Doctor
Consult a physician if:
Pain lasts more than 2–3 weeks
Symptoms worsen
Leg weakness develops
There is unexplained weight loss or fever
Early diagnosis prevents chronicity and long-term disability.
Final Word
Lower back pain can disrupt daily life, but it is rarely untreatable. With early intervention, proper evaluation, lifestyle modification, and structured rehabilitation, most individuals recover completely.
Ignoring persistent symptoms, however, may convert a simple strain into a chronic spinal disorder.
If you or your patients are experiencing recurring lower back pain, a systematic evaluation and individualized management plan is the key to long-term relief.